Question & Answer - Oral Sensory-Motor, Myofunctional, Vocal Tract, & Airway Information
Do nasal breathing-oral breathing work in solidarity?Answer from Dr. Adriana N. Habbaby in ArgentinaJuly 2017 |
|||
|
W The human being benefits from nasal breathing. Physiologically, natural breathing allows the entry of air through the nostrils. Oral breathing, however, appears to be totally inadequate and detrimental due to the symptoms and consequences it causes in children and adults. Mouth breathing syndrome (Segovia, 1988) presents with dry mouth; inflamed gums; high, narrow, palate causing long face syndrome; dental malocclusion (e.g., open bites, dental crowding); tongue in dental interposition; altered body posture; prominent abdomen; winged scapulae; dysfunctional swallowing; snoring during sleep; recurrent otitis media; Eustachian tube dysfunction; pallor; and learning problems (Segovia ,1988). Mouth breathing syndrome
But, can one speak of pure mouth breathing? This is rarely the case because most people use mixed breathing. Often a person breathes nasally diurnal (i.e., during the day) and orally at night because at night the person cannot control the respiratory mode. The degree of obstruction of the upper airway is also influenced by hypertrophic adenoids and/or tonsils, nasal polyps, nasal septum deviation, allergies, sinusitis, short lingual frenulum, etc. Is oral breathing always pathological? NO, since athletes use it when performing certain sports such as swimming. We also perform mouth breathing when singing or speaking. During phonation, the soft palate closes or opens the expiratory air stream for nasal (e.g., English “m, n, and ng”) and oral phonemes. Other languages use nasality differently than English. When we evaluate the phonation of each vowel analyzing how it is performed, we should not hear nasality in the cases of /e/, /i /, /o/, /u/, whereas the /a/ normally has minimal air leakage through the nasal cavity.
A very important fact to take into account is what happens during the nasal cycle. When we evaluate the symmetry of nasal permeability with the Glatzer mirror, we expect the airflow to be identical on both sides to be considered normal. If it is asymmetrical, we need to consider that there is likely an obstruction on the side where we see less air. However, we frequently do not consider the nasal cycle where breathing is alternating between the left fossa and the right fossa. This cycle changes in hours according to age. Older people have a longer period of time for their cycles. To determine with the mirror if a nasal area is obstructed, one nostril is evaluated at a time by obturating or occluding the opposite. The one that has a hissing sound is the one suffering a blockage.
http://www.infoescola.com/sistema-respiratorio/ciclo-nasal/
Glatzer mirror In looking at the etiopathogeny of mouth breathing, we must consider: -Cause of obstruction at the level of the nasopharyngeal airway -Cause of bad habit -Cause of postural alteration What should we do? Look for the cause and how to decrease the negative symptoms. The way we breathe not only alters maxillofacial structures but also modifies brain functioning. If we breathe through the nose we achieve a physiological and psychological balance because breathing is closely linked to emotions such as a sigh of discouragement, crying, gasping in pain, or vocalizing a euphoric state (Habbaby, 2006). Breathing is regulated by a respiratory center at the level of the brain stem which regulates the respiratory rate. Medical treatment may involve: -Medication -Surgery Speech-language therapy for the mouth-breathing patient may encompass: -Promotion of nasal breathing through specific exercises for this purpose -Strengthening the orofacial muscles to improve lip closure -Repositioning the lingual posture to improve the function of the temporo-mandibular joint and swallowing -Improving postural control References Guyton, AC, & Hall, JE (2006). Textbook of medical physiology (11 ed.). Madrid: McGraw-Hill Interamericana. Habbaby, A. (2006). Disfonías del niño y del adolescente. Edit. Akadia. BA Segovia, ML (1988). Interrelaciones entre la Odontoestomatología y la Fonoaudiología. La Deglución Atípica. Editorial Médica Panamericana. Buenos Aires, Argentina
- PhD in Speech, Language, and Audiology Pathology. Graduated from the Faculty of Medicine of the University of Salvador and PhD from UMSA (University of the Argentine Social Museum). Bs As. Argentina -Specializes in speech, language, audiology, and stomatology at the Hospital Cosme Argerich.de Buenos Aires. Argentina. Otorhinolaryngology Unit -Professorship participation in the Chair of Vocal Pathology I, Speech Therapy career at the UBA and in the Department of Teaching and Research at Cosme Argerich Hospital -Professor of courses at distance and presence C.I.Fo.- Training and Exchange in Speech-Language Pathology and Audiology for 10 years -In 2012, she completed her rotation at the Lakeshore Professional Voice Center and School of Medicine, Wayne State University, Detroit, Michigan, USA -More than 28 years of experience working with speech, stomatology, language, and audiology pathologies in babies, children, and adults -Author of the books: Enfoque integral del niño con fisura labio palatina, Edit. Médica Panamericana. Bs As. (2000); Arg. Disfonias del niño y del adolescente. Edit. Akadia (1° 2006)-2° editc. 2017. Bs As. Arg; Co-author: Clínica Fonoaudiológica. Edit. Univer. Rosario. Arg. (2010) -Author and co-author of research papers and books on topics related to the voice, speech, and stomatology problems for Argentina-México y Brazil |
|||
 e know that breathing is a vital element in human life. The respiratory system is responsible for receiving and sending oxygen to all tissues of the body.
e know that breathing is a vital element in human life. The respiratory system is responsible for receiving and sending oxygen to all tissues of the body.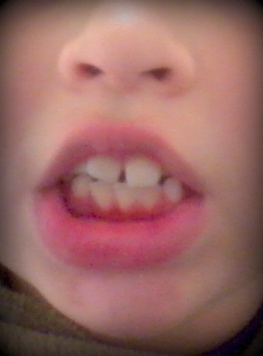 At some point when the airway is obstructed, the respiratory habit changes from nasal to oral resulting in forced breathing. At first this can be intermittent until the habit is set and becomes chronic. The consequences of this type of respiratory function are listed above.
At some point when the airway is obstructed, the respiratory habit changes from nasal to oral resulting in forced breathing. At first this can be intermittent until the habit is set and becomes chronic. The consequences of this type of respiratory function are listed above.




 About Dr. Adriana Nora Habbaby (
About Dr. Adriana Nora Habbaby (